Scabies vs eczema can be a bit of a head-scratcher because they both cause rashes and itching. It's easy to get them mixed up, which can lead to a whole lot of trial and error with treatments. Knowing the difference between them is really important for getting the right help. So, keep on reading to learn more about what sets these skin conditions apart and how to deal with each.
What is Scabies?
Scabies is this annoying skin problem caused by teeny-tiny mites. The pathogen got its name from the Greek, meaning to gnaw meat. These mites love the cooler weather because they survive better when it's not too hot. When it's cold, people sweat less, and our skin isn't as good at fighting off these mites. That's why scabies often pop up more in the colder seasons.
When you have scabies, you'll probably feel super itchy, especially at night. You might notice rashes with red spots and little lines where the mites have tunneled under the skin. This can happen all over, but common spots are on the wrists, elbows, armpits, waist, private parts, buttocks, and between your fingers. There are a few types of scabies: typical scabies, nodular scabies, and Norwegian scabies.
Types of Scabies
- Typical Scabies: This one's the most common. It gives you itchy rashes that can pop up pretty much anywhere but your face or scalp. The rashes look like small red bumps, all clustered together.
- Nodular Scabies: Here, you get a few itchy bumps that are red, pink, or brown, usually around your private areas, armpits, or groin. Sometimes, these bumps are the only way to tell it's scabies.
- Norwegian Scabies: This is the serious stuff, mostly hitting people with weaker immune systems. It leads to thick crusts on your skin because there are a ton of mites involved.
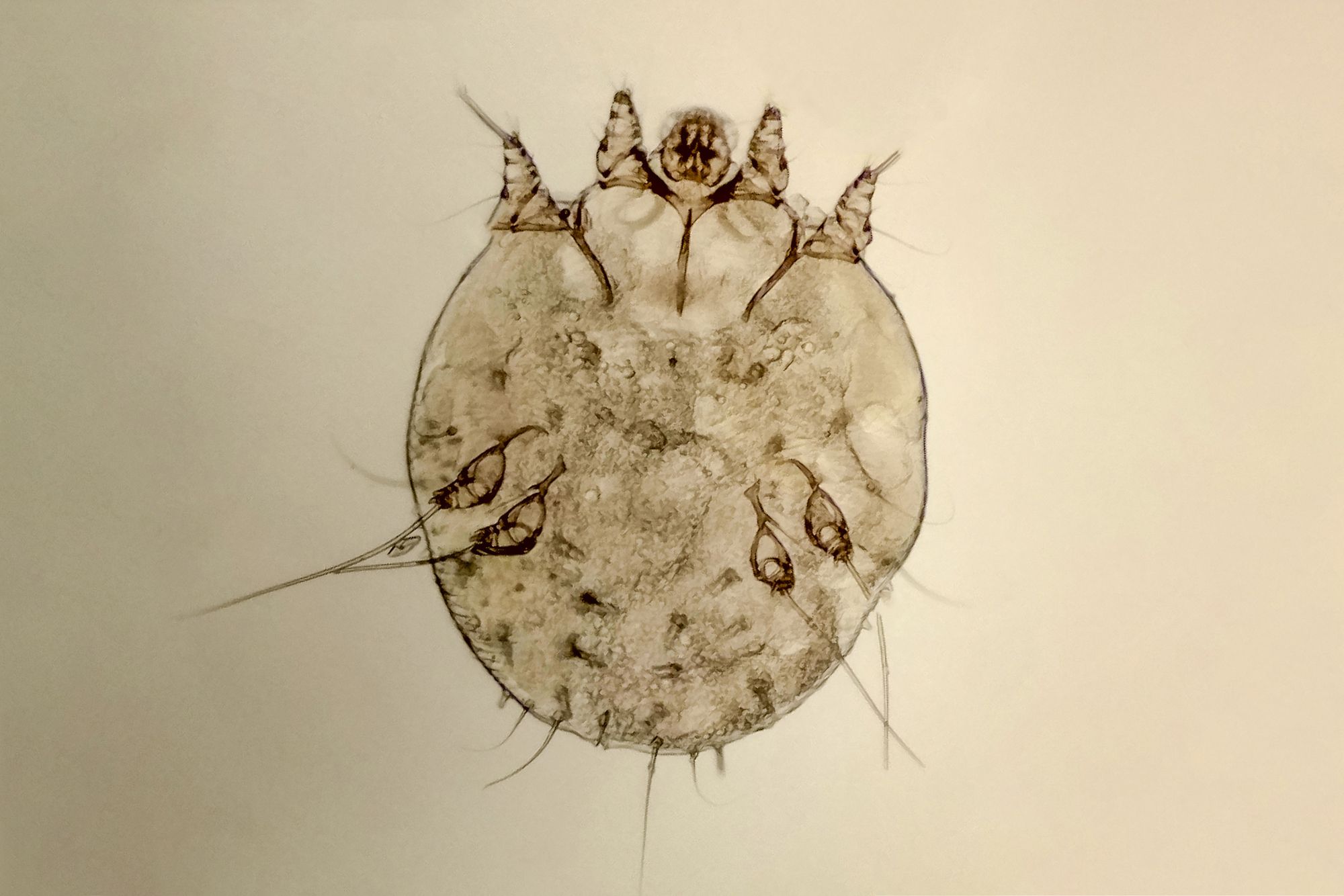
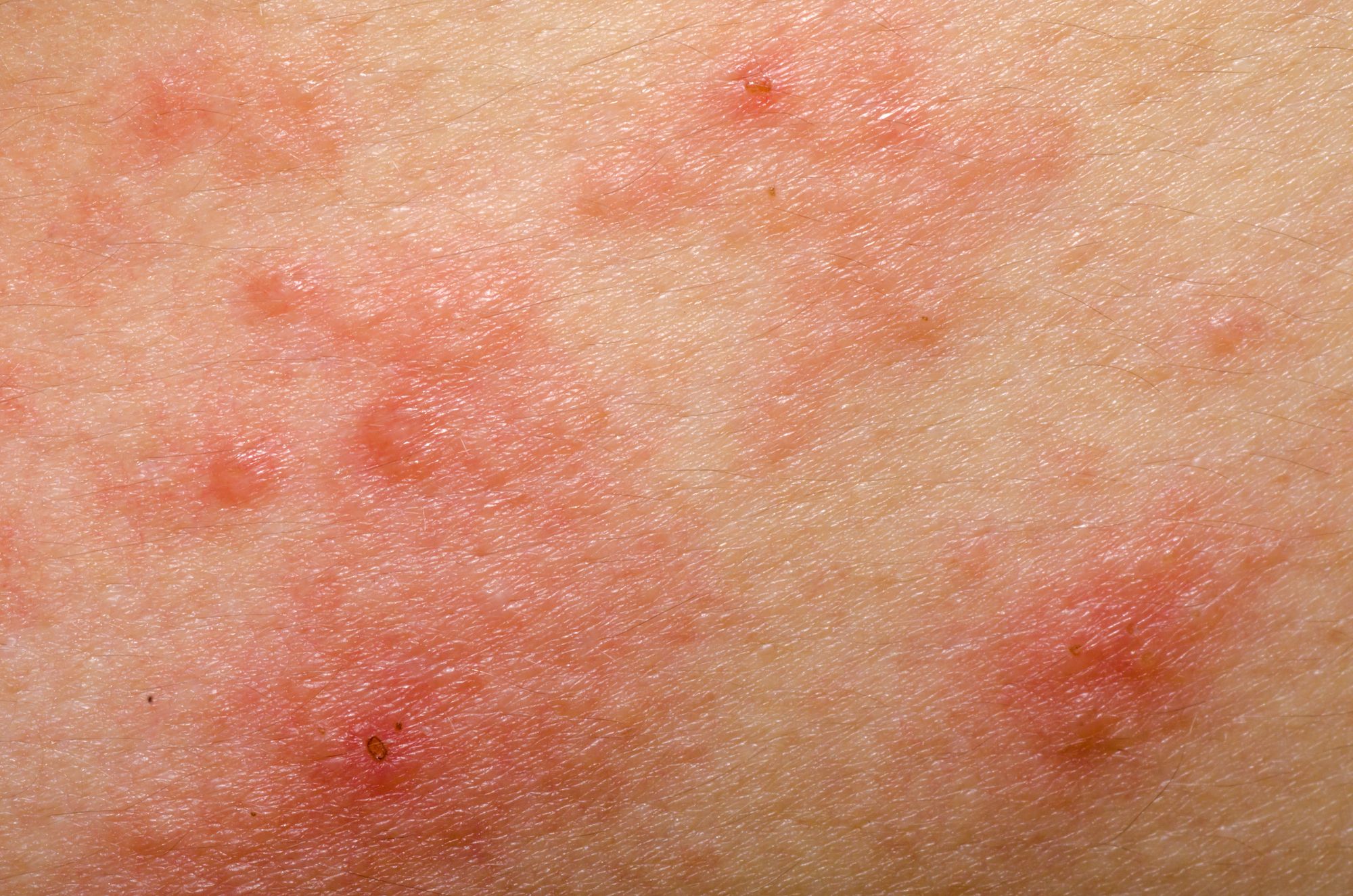
Mite (left) & Scabies Rash (right)
What is Eczema?
Eczema is a long-term skin issue that makes you itchy and gives you red rashes and tiny blisters. No one's totally sure why people get it, but it might be something to do with your genes and stuff around you, like irritating chemicals, allergies, and even stress. There are seven kinds of eczema: atopic dermatitis (the most common one), discoid eczema (round patches), neurodermatitis (thick, scaly patches), dyshidrotic eczema (blisters on hands and feet), contact dermatitis (from touching irritants), stasis dermatitis (usually on lower legs), and seborrheic dermatitis (oily, scaly skin).
Types of Eczema
- Atopic Dermatitis: This is a long-term type of eczema that often starts when you're a kid and usually gets less annoying as you grow up. It's super common in babies – like 85% of their skin rashes are this kind. It's pretty much an allergy thing and is linked to other immune issues.
- Discoid Eczema: This one makes round, disc-shaped patches on your skin. It's itchy, and the skin gets inflamed. Sometimes, these patches have a clear center with a red ring around it.
- Neurodermatitis: This chronic skin condition can be linked to both nerves and allergies. It starts with itching and then turns into thick, scaly patches.
- Dyshidrotic Eczema: This shows up as itchy blisters on your hands and feet. It can be really sore and make it hard to use your hands or walk.
- Contact Dermatitis: You get this from touching certain stuff. It starts as itchy red skin with little bumps, usually right where you touched the irritant or allergen, and can spread from there.
- Stasis Dermatitis: This happens on your legs if you have ongoing issues with blood flow there. It can itch, flake, and make your skin change color.
- Seborrheic Dermatitis: Affecting areas with a lot of oil glands, this causes itchiness, dandruff, and oily yellow scales.
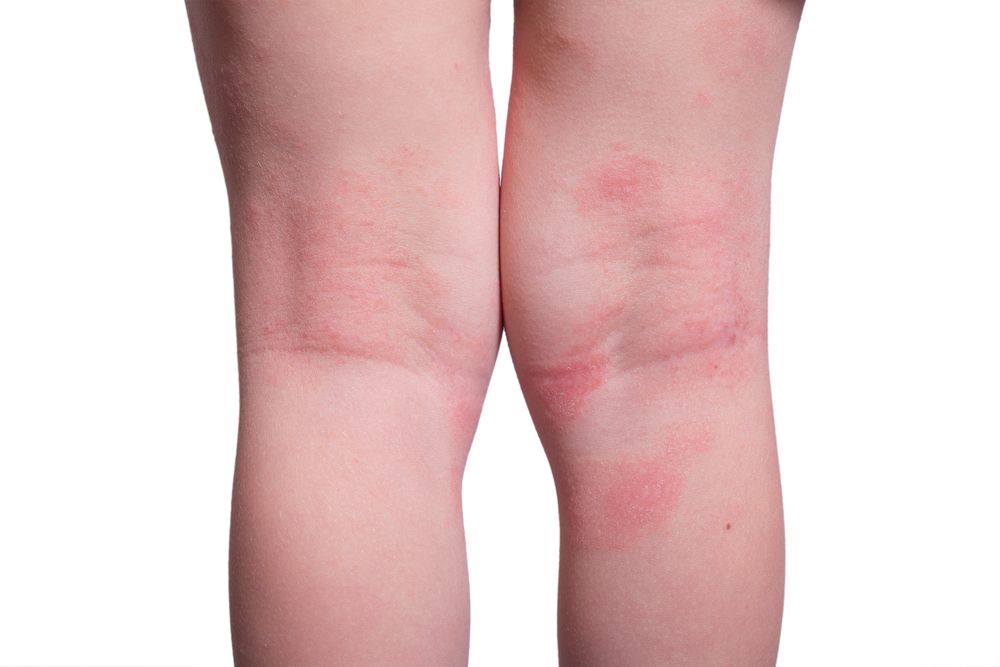
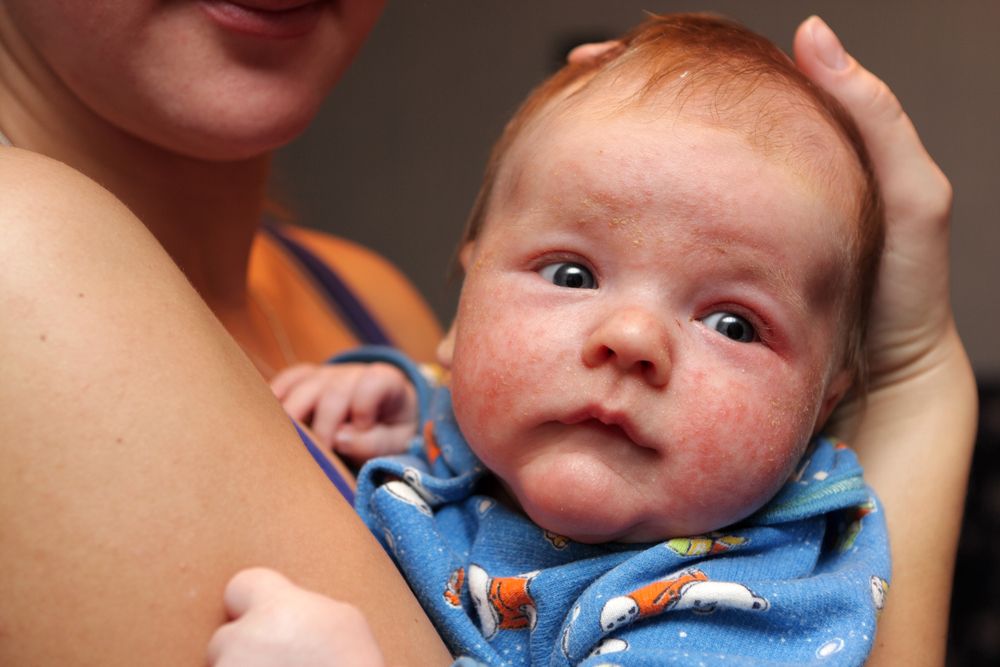
Scabies vs Eczema
Causes
- Scabies: This happens because of a tiny parasite called the Sarcoptes scabiei mite. These mites burrow into the top layer of your skin to live and lay eggs, and they can stick around for months if you don't treat them.
- Eczema: This one's triggered by a bunch of stuff like rough soaps, strong detergents, and heavy shampoos. Also, the environment plays a role – think bad weather, too much moisture, or super dry air. And don't forget allergens like house dust, pet hair, and molds.
Contagiousness
- Scabies: Super contagious! It spreads if you're in close, skin-to-skin contact with someone who's got it for a while. But don't worry, it doesn't catch on with just a quick touch or a hug.
- Eczema: No stress here – it's not contagious at all. You can't catch it or pass it on to someone else.
Symptoms
- Scabies: You'll usually see signs 2-5 weeks after you've been around someone with scabies. The big giveaway? Really itchy skin at night and a rash with bumps that look like tiny tunnels. Watch out for it on wrists, elbows, armpits, nipples, waist, private parts, buttocks, and between fingers. Scratching a lot spreads the mites to new areas, and if you don't treat it, it can get worse and even cause infections.
- Eczema: This also makes you itchy, but it can pop up anytime (allergic contact dermatitis is the exception). Eczema's rash looks like small, inflamed blisters and can spread all over. The more you scratch, the itchier it gets.
Diagnosis
- Scabies: The easiest way to check for scabies? Put some iodine on the itchy skin and see if there are any burrow-like lines. Or, doctors can use a fancy tool called a digital dermatoscope that magnifies the skin 600 times to spot scabies almost every time.
- Eczema: To figure out if you have eczema, doctors do a few things. They'll look at your skin, ask about stuff you've touched recently that might irritate your skin or cause allergies, take a blood sample, and sometimes even take a tiny bit of skin for testing.
Treatments
- Scabies: The main goal is to kill the mites and stop them from coming back. Your doctor will probably give you something with sulfur to wipe out the mites. After a hot bath or shower, you'll need to slather this all over your body, even under your nails (since mites like to lay eggs there when you scratch). Even after the mites are gone, you might still itch and have a rash for a few weeks. To help with this, you might use Hydrocortisone 1% and Antihistamine creams.
- Eczema: The key here is figuring out and avoiding what triggers your eczema. Depending on your eczema type, your doctor will suggest a plan. Usually, this includes antihistamines in combination with topical agents (anti-itching and anti-irritation creams) and repairing balm to restore damaged moisture barrier.

